Engaging Providers Key to Value-Based Reimbursement Adoption
With 73 percent of surveyed providers favoring fee-for-service, researchers advised leaders to boost provider engagement for robust value-based reimbursement adoption.

Source: Thinkstock
- Nearly three-quarters (73 percent) of providers prefer a fee-for-service model over value-based reimbursement structures even though almost one-half acknowledged that the traditional payment model contributed to higher healthcare costs, a recent Bain & Company survey showed.
The survey of 980 physicians and 200 healthcare finance and procurement officers showed that providers are not convinced that value-based reimbursement models will improve care quality enough to offset declining healthcare costs.
As a result, about 65 percent of physicians anticipated high-quality care to be significantly more difficult to deliver in the next two years. Physicians cited complex healthcare regulations, additional administration burdens, and a complicated reimbursement landscape as the reasons why.
Another 53 percent said that capitation payments would decrease care quality and 21 percent stated that they do not see many care quality benefits from pay-for-performance models.
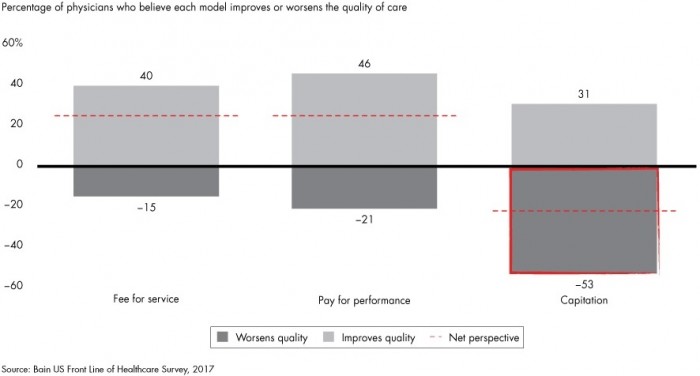
Source: Bain & Company
However, researchers found that engaging providers may be the key to value-based reimbursement adoption.
“Our survey findings indicate that bringing physicians back into the decision-making process helps create greater momentum for change,” the report stated. “Physicians who are not aligned and engaged with their organizations have more reasons to resist new structures and systems, such as value-based payment models.”
“By contrast, those who have a say in management decisions are much more satisfied with their working environment and more willing to lead change,” researchers added.
Provider resistance to value-based reimbursement adoption slowed the transition away from fee-for-service payments across organization types. Providers in the 2015 survey expected a broad value-based reimbursement adoption rates.
However, Bain researchers found that most healthcare organizations have reached a plateau with their value-based reimbursement adoption efforts after five years of rapid payment and health IT change.
The results echoed the findings from a recent AMGA survey. The survey showed that healthcare leaders in 2015 thought just 68 percent of their 2016 commercial revenue would come from fee-for-service.
However, respondents reported in 2016 that 77.3 percent of their commercial revenue stemmed from a fee-for-service payment model.
Despite provider reluctance to adopt value-based reimbursement models, the Bain survey showed that healthcare organizations are engaging with a mix of fee-for-service and alternative payment models to comply with industry-wide value-based reform goals. HHS expects to tie 90 percent of traditional Medicare reimbursement to a value-based reimbursement model by the end of 2018.
To meet value-based reimbursement adoption goals, healthcare organizations should allow providers to participate in the move away from fee-for-service.
The provider engagement approach is particularly important since almost 60 percent of providers agreed that their facilities were not ready for value-based reimbursement adoption because they lacked aligned organization and clear accountabilities.
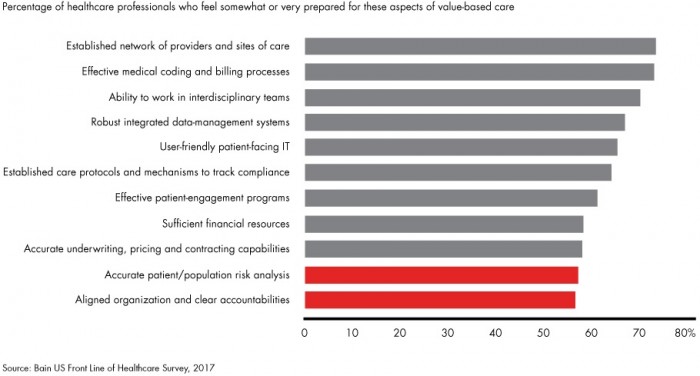
Source: Bain & Company
The engagement strategy proved effective in earning surgeon buy-in with healthcare cost reduction initiatives, the survey stated.
Many healthcare organizations employed procurement professionals for healthcare supply chain management. Procurement staff aimed to maximize healthcare supply chain budgets, but surgeons frequently clashed with the staff over supply needs.
However, allowing surgeons to participate more in the healthcare supply chain management process boosted provider perception of procurement staff. With more than 80 percent of surgeons collaborating with procurement staff in 2017, about 43 percent the providers viewed the procurement department as an effective tool for improving care quality and decreasing costs.
“Physicians who are not aligned and engaged with their organizations have more reasons to resist new structures and systems, such as value-based payment models,” the report explained. “By contrast, those who have a say in management decisions are much more satisfied with their working environment and more willing to lead change.”
Healthcare leaders should look to provider-led organizations to improve provider engagement strategies, researchers added.
About 80 percent of physicians in provider-led organizations felt inspired by their organization’s mission and another 83 percent said they were sufficiently engaged in strategic decision-making.
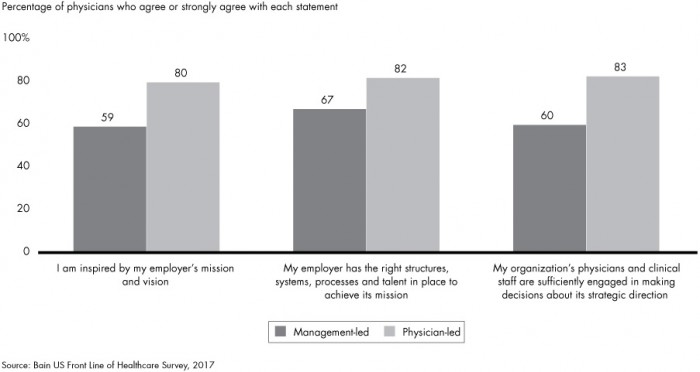
Source: Bain & Company
In contrast, only 59 percent of providers in management-led organizations felt inspired and just 60 percent felt sufficiently engaged.
Researchers also advised healthcare organizations to promote both clinical and financial benefits of value-based reimbursement adoption to spur more provider backing.
“Physicians need a clinical rationale for changing the way they deliver care—financial logic alone will not change long-established behaviors,” the report stated. “Indeed, many have overlooked the role of the physician as system innovator. Physicians tell us that they are open to new cost-saving models, but need to be on the front line of change helping health systems identify which approaches create value for patients, and which don’t.”
