85% of Orgs Looking to Replace Revenue Cycle Management Systems
More healthcare organizations are seeking revenue cycle management solutions that can accommodate the needs of value-based reimbursement models, Black Book says.

- Eighty-five percent of provider organizations, hospitals, and physician practices are currently seeking to replace their healthcare revenue cycle management systems or are deciding if it is time to switch, according to a new survey from Black Book Market Research.

In the survey of more than 5000 revenue cycle professionals, ninety-three percent said that they need to do away with revenue cycle management, financial, and coding technology vendors that have not generated a return on investment by the end of the year. Only 79 percent of CFOs reported the same thing in the fourth quarter of 2015, indicating an increasing urgency to achieve ROI.
“As reimbursements come under pressure and costs keep rising, provider CFOs will face unparalleled pressure over the next year to preserve financial solvency, increase productivities in care delivery, implement regulatory mandates and reduce RCM [revenue cycle management] expenses associated with getting paid,” said Doug Brown, Managing Partner of Black Book
New or updated systems would lead to better financial health and increased efficiency, according to 94 percent of healthcare CFOs. However, nearly half (48 percent) are concerned that organizational budgets will prevent them from implementing end-to-end revenue cycle management systems that they need for succeeding under changing reimbursement structures in 2017.
New value-based reimbursement structures are also driving replacement projects, stated the survey. With 94 percent of surveyed hospitals getting paid under a mix of value-based care and fee-for-service contracts in the third quarter of 2016, many are seeking revenue cycle management solutions that offer more accountable care functions.
Ninety-three percent of healthcare CFOs are looking for “financial functionality” in solutions that include population health, coding, analytics, forecasting, budgeting, and alternative payment models.
“Healthcare providers will have no choice but to evaluate and optimize their RCM solutions end-to-end in a future state that leverages analytics and enhanced connectivity with payers, all keeping pace with the advances in healthcare technology,” said Brown.
End-to-end revenue cycle management solutions that manage the process from patient intake to claims reimbursement have improved the bottom lines for many providers, including outsourced and software options, the survey showed. Revenues increased by 8.1 percent for physician practices that outsourced the process and 5.5 percent for physician practices that worked with a software vendor. For hospitals, revenue rose by 8.4 percent with an outsourced solution and 14.4 percent with a software vendor.
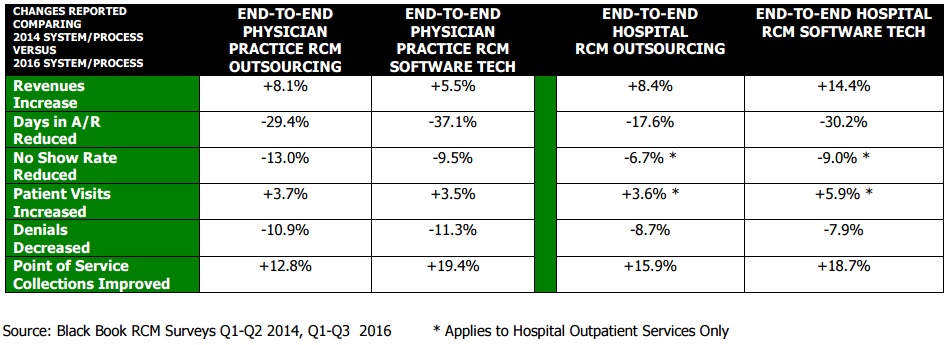
Researchers reported that outsourcing and bolt-on technologies for existing systems have become a popular option for provider organizations looking to replace their vendors and programs.
While 29 percent of hospitals are using an advisor or consultant to manage revenue cycle management transition activities, 71 percent of those providers have not chosen an end-to-end technology vendor.
As a result, more providers are outsourcing all or key parts of healthcare revenue cycle management or investing in bolt-on technologies for their current systems. Seventy percent of medical group practices who are collaborating with consultants are thinking of outsourcing revenue cycle management solutions in 2017.
While outsourced solutions rose nearly two-fold between January 2015 and August 2016 for key revenue cycle management functions, 77 percent of hospital CFOs see it as a temporary solution until new software is implemented.
Outsourcing is considered an ongoing solution for the next 18 to 36 months for 60 percent of small, rural, and large hospitals as well as 70 percent of community hospitals.
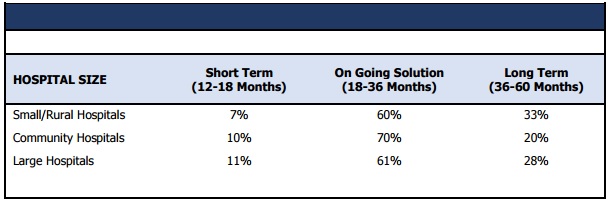
However, Black Book pointed out that some providers are trying to implement in-house systems to keep control of their revenue cycle. Eighty-seven percent of self-determined profitable hospitals said that they are keeping their software and personnel within the organization. In addition to retaining control, in-house solutions produce a better return on investment after training employees and upgrading technologies, participants noted.
Despite the large push to replace revenue cycle management solutions, the survey indicated that the desire for new tools may not necessarily translate to action. Almost one-third of hospitals that thought they would replace their solutions in 2016 have not yet initiated the project.
Similar to the 2013 Black Book survey, researchers also reported that hospital executives prioritize revenue cycle management replacement projects differently. While 70 percent of CIOs and 92 percent of CFOs agree that revenue cycle management solutions need to be updated, evaluated, outsourced, or replaced, the project’s implementation plan, timing, and prioritization differ among the executives.
Additionally, the 2016 survey revealed that enterprise integration with current clinical systems is no longer the primary motivator for vendor decisions, except in small hospitals.
Providers are more concerned with how vendors respond to smaller margins, higher costs, and Medicare reimbursement reductions, as well as new payment contracts that require increased efficiencies and automation.
Researchers also identified the top ranked end-to-end revenue cycle management software and technology vendors from the past year.
The end-to-end vendors with the highest client satisfaction and loyalty rates in 2016 were as follows:
• Navicure for small, rural, and critical access hospitals with fewer than 100 beds
• Advisory Board for community hospitals with 101 to 200 beds
• ZirMed for large hospitals with over 200 beds (fifth consecutive win)
Other vendors with top scores among hospitals include Cerner/Siemens, Conifer Health, Recondo Technology, Availity, and Rycan.
Among outsourcing end-to-end revenue cycle management vendors, Optum360 took first place among hospital managed system corporations, systems, networks, and chains for the third consecutive year. nThrive (formerly MedAssets & Precyse) ranked highest among small and community hospitals, while Conifer Health was the most popular with large hospitals.
“As RCM transformation disruption accelerates, the top rated vendors are allowing providers access to the expertise to structure systems and processes that contribute to their unique financial imperatives and strategic goals,” Brown stated. “What was once considered a back office function just a few years ago, has evolved into a full end-to-end system that begins even before patient registration.”
Image Source: Black Book Market Research
Dig Deeper:
• What is Healthcare Revenue Cycle Management?
• Preparing the Healthcare Revenue Cycle for Value-Based Care
