CMS Tackles Medicare Spending, Medicaid Financial Incentives
Misaligned provider incentives hinder Medicare and Medicaid spending. CMS says dual enrollees demand better alignment and cohesiveness across the two programs.

- Medicare and Medicaid spending demands closer alignment for healthcare providers to better manage costs, according to a new report from the Centers for Medicare & Medicaid Services (CMS).

A CMS/state partnership Capitated Model and the Managed Fee-for-Service Model under the Medicare-Medicaid Financial Alignment Initiative tests integrated care models for Medicare-Medicaid enrollees.
The overarching goal is to develop person-centered care delivery models via joint incentives that fully integrate medical, behavioral health, and long-term services.
The Initiative – executed under the CMS Innovation Center and the CMS Medicare-Medicaid Coordination Office – also promotes a high quality care experience for dual eligible Medicare-Medicaid enrollees.
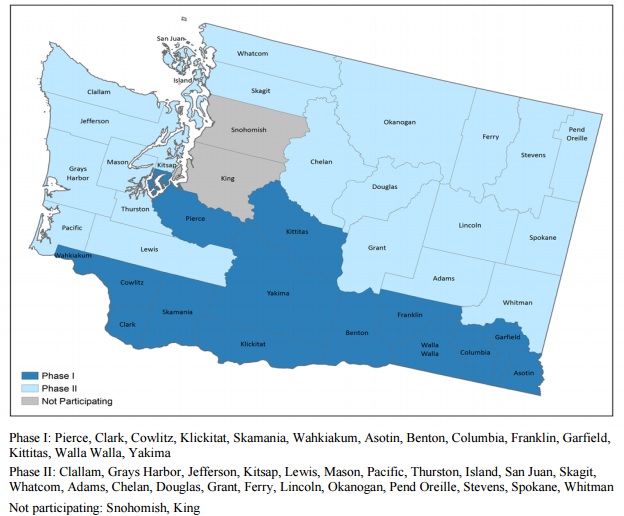
A key focus under the Initiative’s Washington Health Homes demonstration is on coordinated services across Medicare and Medicaid for Washington State Medicare-Medicaid enrollees and shared savings. The big focus is on improving quality while keeping costs low.
“A longstanding barrier to improving quality and reducing costs of care for Medicare-Medicaid enrollees has been a lack of alignment and cohesiveness between the two programs, including misaligned incentives for payers and providers,” writes Patrick Conway, MD, CMS Principal Deputy Administrator and Chief Medical Officer.
“CMS is developing a centralized system to implement [alignment] principles consistently across initiatives while recognizing the rules and methodologies of each shared savings initiative,” CMS asserts.
The Affordable Care Act (ACA), says CMS, has generated opportunities for healthcare providers to participate in various new models of care to help lower costs.
“The success of any care coordination initiative -- including Financial Alignment Demonstration models -- depends on creating new care delivery models that significantly improve the care that beneficiaries receive.”
CMS report details 2013-2014 Medicare spending data
“Despite the relatively short time period, estimates show a reduction of $21.6 million in Medicare spending relative to a comparison group, representing more than 6% savings,” Conway explains.
“While these findings are preliminary, they provide an encouraging first look at how efforts in Washington to improve quality of care by focusing on the needs of high-risk, high-cost members can reduce Medicare spending.”
A first annual evaluation report on the Washington demonstration is planned for release later this year. The report will detail cost measures for Medicare-Medicaid enrollees eligible for both the demonstration and a comparison group, Conway states.
“This model further supports delivery system reform aimed at achieving better care, smarter spending, and healthier people. It is especially important to focus on the safety net population served by this model in order to reduce disparities and coordinate care for vulnerable populations.”
The fee-for-service initiative
The Department of Health and Human Services (HHS) announced Washington as the first state to join CMS in October of 2012. Washington and CMS planned to test a managed-fee-for-service model for providing Medicare-Medicaid enrollees with a more coordinated, person-centered care experience.
“Through the demonstration, Washington is building upon its Medicaid health home model, targeting Medicare-Medicaid enrollees with chronic health conditions,” CMS says.
Massachusetts became the first state to enter a Memorandum of Understanding (MOU) with CMS to test the capitated Financial Alignment model. The other states with an MOU are: California, Colorado, Illinois, Michigan, Minnesota, New York, Ohio, South Carolina, Texas, and Virginia.
“Improving the care experience for low-income seniors and people with disabilities who are Medicare-Medicaid enrollees – sometimes referred to as 'dual eligible individuals'– is a priority for CMS,” said the organization.
“Many Medicare-Medicaid enrollees suffer from multiple or severe chronic conditions and could benefit from better care coordination and management of health and long-term services and supports.”
