Hospital Mergers Take Two or More Years to Produce Cost Savings
Organizations may see immediate cost reductions after a hospital merger, but falling operating margins offset savings for about two years after the transaction, a study showed.

Source: Thinkstock
- Hospital mergers and acquisitions resulted in immediate decreases in operating expenses per adjusted admission. However, acquired facilities also saw operating revenue decline at a higher rate, leading to falling operating margins for the first two years after the transaction, a recent Deloitte and Healthcare Financial Management Association (HFMA) report showed.
Merger and acquisition activity among hospitals has steadily increased in the last decade. Nearly 400 hospital mergers and acquisitions transactions occurred between 2008 and 2014, with more than 750 hospitals being acquired or merged, the analysis showed.
Hospitals and health systems are looking to mergers and acquisitions for financial, operational, and strategic value, revealed a Deloitte and HFMA survey of 90 hospital financial executives from merged or acquired organizations and phone interviews with 13 healthcare leaders.
The ability to boost market share was the top reason for hospital mergers and acquisitions, according to 40 percent of executives from acquirer hospitals or health systems.
The organizations aimed to increase market share to broaden its physician network and increase its patient outreach, which would help the hospital or health system engage in two-sided financial risk models.
READ MORE: Do Hospital Mergers Disincentivize Orgs to Lower Their Costs?
For acquired entities, access to capital was the primary driver for hospital merger and acquisition activity. About 31 percent stated additional capital was the top driver for pursuing an acquisition.
While acquirer and acquired organizations sought a hospital merger or acquisition for different reasons, executives from both sides of the transaction agreed that delivering care more efficiently was a top driver. Approximately 24 percent of acquirers and 29 percent of acquired entities selected more efficient care as a primary reason.
Cost efficiency may have been a goal for acquired and acquirer organizations, but the analysis and survey results showed that hospitals and health systems may not realize financial improvements until two years after the transaction.
Declining operating revenue per adjusted admission and overall hospital operating margins did not start to level off until two years after the transaction.
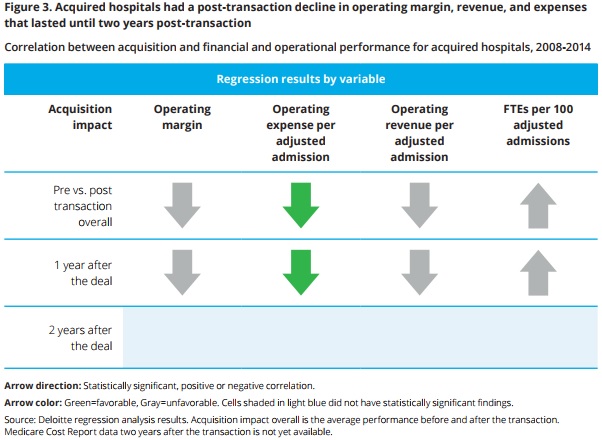
Source: Deloitte, HFMA
Executives attributed lackluster financial and operational results to immediate investments as part of the hospital merger and acquisition as well as additional staffing needed to improve care quality at the acquired facility.
READ MORE: Key Strategies for Health Systems to Achieve Economies of Scale
Despite falling operating margins, hospital and health system leaders reported that hospital merger and acquisition transactions did reduce healthcare costs after several years. Roughly 40 percent of respondents stated that their organization met 25 percent of their cost-structure efficiency goals.
Although, the organizations that did achieve their financial goals reported that it took over two years for improvement initiatives and investments to pay off.
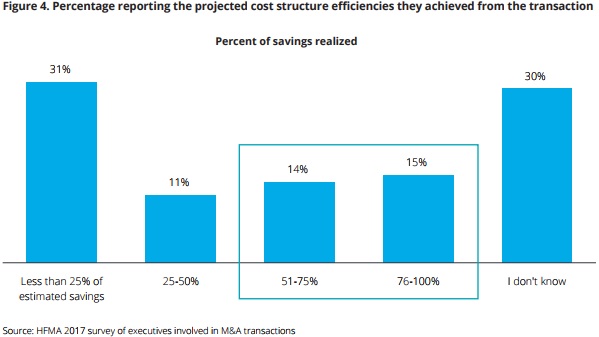
Source: Deloitte, HFMA
Financial and operational improvements may have taken time to realize, but nearly 80 percent of executives said that the acquired organization made significant capital investments post-transaction.
About two-thirds of executives stated that health IT or facility upgrades were the top use of new capital invested in acquired organizations.
Thirty-seven percent of respondents said implementing a single health IT system or upgrading existing systems occurred post-transaction and 33 percent reported new capital went to renovating, expanding, or building an acute facility.
READ MORE: Preparing the Healthcare Revenue Cycle for Value-Based Care
Other common uses for new capital included acquiring physician practices with 30 percent of participants, renovating or building ambulatory care sites with 27 percent, implementing or upgrading administrative IT systems with 24 percent, and investing in new movable medical equipment with 17 percent.
How to maximize value from hospital merger and acquisition transactions
The analysis and survey results showed that hospital merger and acquisition value varied by organization, with some taking longer than others to see financial and operational improvements.
Almost one-half of acquired hospitals saw care quality improvements and another 25 percent met at least one-half of the transaction’s cost savings goals.
But 17 percent of executives stated that their transactions accomplished both care quality advancements and achieved cost savings goals.
Researchers found that hospitals and health systems that experienced these high-value hospital mergers shared the following characteristics:
• Established a strong strategic vision for seeking the transaction
• Created explicit financial and non-financial goals
• Held leadership accountable, particularly at the vice president level, for integration initiatives
• Pinpointed cultural differences between acquired and acquirer organizations
• Made upfront and clear decisions regarding executive and middle management leadership
• Aligned clinical and functional leadership early during the hospital merger and acquisition process
• Implemented best practices for integrating an acquired or merged entity into the parent organization
• Developed project management best practices that tracked goals and milestones from the close of the transaction until two years after
Executives also emphasized that integrating the entities is key to engaging in a hospital merger and acquisition that generates higher care quality and cost savings. The top suggestion for improving transaction results was creating an integration plan that aligns with the deal’s strategic rationale.
About 59 percent of leaders involved in a high-value hospital merger and acquisition stated that their organization spent enough time on integration planning and 100 percent said they spent adequate time on integration execution.
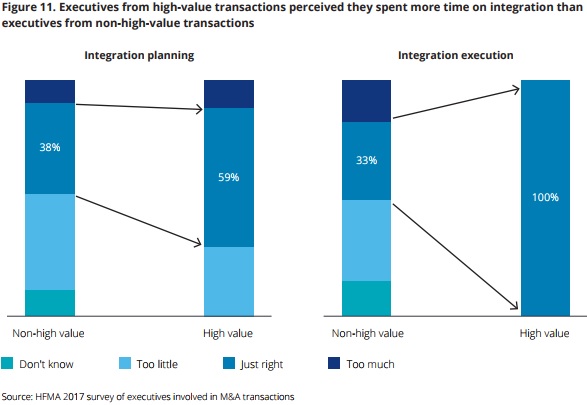
Source: Deloitte, HFMA
In contrast, just 38 percent of executives from non-high-value transactions reported spending enough time on integration planning and only one-third said they spent adequate time on execution.
To improve the integration process, hospitals and health systems should identify integration team leaders early in the merger process. The integration specialists should identify possible challenges and implement integration plans.
Interviewees recommended that executives seek an experienced advisor from outside the organization.
Clear and consistent communication was the next most popular recommendation for increasing transaction value.
Interviewees advised hospital and health system leaders to have pre-hospital merger discussions that address cultural differences. The conversations should also address sensitive topics, such as how much authority the acquired entity’s board will have, identifying executive roles in the combined organization, defining decision-making authority at each level of the merged organization, and pinpointing high-level strategies for redistributing major service lines.
They also suggested that hospital and health system leaders continue the transparent, proactive communication strategy on a scheduled basis. Sixty-five percent of executives from organizations that experienced a high-value hospital merger reported that their organization’s communication was effective versus just 36 percent of executives involved in non-high value transactions.
Having regularly scheduled conversations as well as allowing for organic discussions is crucial to carrying on a communication strategy that will improve hospital merger results.
