The Affordable Care Act’s Effect on Hospital Charity Care

- Hospitals provide charity care according to patients’ income levels. But policies and patient criteria often vary depending on the particular hospital. Supporting hospital charity care while maintaining tight margins is a challenge, especially when healthcare reform roadblocks get in the way.

The Affordable Care Act (ACA) mandated nonprofit hospitals meet several requirements in order to meet their tax exempt standing.
These requirements include limiting the cost of medically necessary care for those eligible for financial assistance and ensuring a patient’s assistance eligibility status early on. But the mandates are perhaps too vague to be effective.
The proposed regulations also do not necessarily determine who is eligible for financial assistance. Hospitals are then left to independently create their own criteria.
This widespread lack of standardization may harm hospital revenue cycle management.
Charity care amounts dropped with Medicare expansion
Charity care complications also arose when some states decided not to partake in Medicaid expansion.
Between 2013 and 2014, inpatient hospital stays for uninsured patients in expansion states dropped by over 44 percent, confirmed the Kaiser Family Foundation.
In states that did not adopt expansion, inpatient stays rose by nearly 6 percent.
For the 26 states that opted to expand Medicaid eligibility, the number of uninsured patients reportedly dropped by over one-third, according to the Robert Wood Johnson Foundation.
Hospitals in expansion states apparently experienced significant reductions in charity care.
The amount of average charity care per hospital across expansion states dropped by 30 percent from $2.8 million to $1.9 million, confirmed 2014 research from the Colorado Hospital Association.
Among expansion states, self-pay charges reportedly dipped by 25 percent.
There was no reported change in charity care, Medicaid, and self-pay aside from normal variation across non-expansion states.
Medicaid, self-pay and charity care showed no change outside normal variation for hospitals in non-expansion states in 2014.
“This decline in self-pay and charity care, occurring in parallel with the growth in numbers of Medicaid beneficiaries, shows that previously uninsured patients are now enrolled in Medicaid,” the report stated.
“Many hospitals provided on-site assistance to enroll eligible patients into Medicaid, promoting the recruitment of patients into Medicaid who otherwise would have self-paid or been provided with charity care.”
One-fourth of 340B hospitals provide charity care
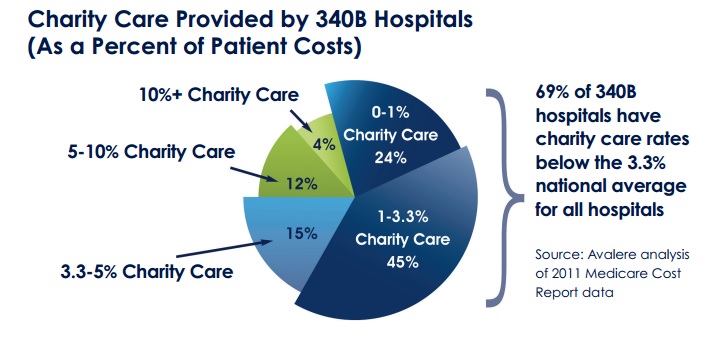
About one-fourth of 340B hospitals provide charity care representing no greater than 1 percent of their total patient costs, according to the Alliance for Integrity and Reform (Alliance).
Charity care represents a fairly large share of patient costs, but only for relatively few 340B hospitals.
“For more than two-thirds of 340B hospitals, charity care as a percent of patient costs is less than the national average of 3.3% for all hospitals,” the Alliance stated.
“[Less] than a third of 340B hospitals are providing more charity care than the average for all hospitals combined – including for-profit hospitals.”
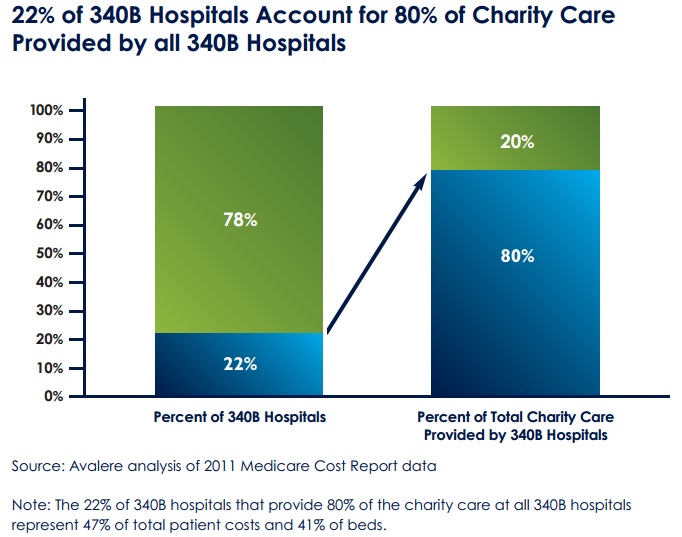
Nearly “one-fifth of 340B hospitals provide 80% of all charity care delivered by 340B hospitals, even though these hospitals account for less than half of all 340B hospital beds.”
As hospitals and healthcare providers struggle to provide quality care to their most financially strapped patients, it is hopeful more standardization across the industry for eligibility criteria will keep the focus on care instead of cost.
Image Credits: The Alliance for Integrity and Reform
