New Alternative Payment Model Tackles Holistic Addiction Recovery
A national alliance created an alternative payment model that will use risk- and value-based reimbursement to align clinical and economic incentives for improved addiction recovery care.

Source: Thinkstock
- A national multi-sector alliance of healthcare industry leaders is looking to incentivize providers and payers to deliver coordinated, holistic addiction recovery services to patients through a new alternative payment model.
Nearly 21 million people have a substance abuse disorder. Yet only one out of ten individuals receive treatment, according to data from the Surgeon General.
To combat the substance abuse crisis impacting about one in three households, Leavitt Partners, Facing Addiction with NCADD (The National Council on Alcoholism and Drug Dependence), Remedy Partners, and other groups recently developed the Addiction Recovery Medical Home model.
The alternative payment model aims to financially incentivize providers, payers, and other addiction recovery stakeholders to treat individuals with substance abuse disorders as if they had a chronic condition.
The healthcare system currently treats chronic conditions using “standards of excellence,” the alliance explains. The standards inform consumers, health systems, and payers about best practices for treatment and services that should be delivered to patients.
READ MORE: Key Capabilities for Population-Based Alternative Payment Models
The standards of excellence promote long-term, coordinated care for individuals with chronic conditions and many payers, including Medicare and Medicaid, offer providers the financial incentives to deliver chronic disease management through alternative payment models.
However, individuals suffering from alcohol and drug addictions typically receive fragmented care that spans the emergency department, addiction treatment centers, community health organizations, and other care settings. Despite the long-term, coordinated care needed, providers oftentimes cannot bridge the gap between physical, behavioral, and community health to deliver high-quality addiction recovery treatment to their patients. Technological, regulatory, and payment barriers also exist that prevent coordinated care for substance abuse disorders.
The national alliance led by Leavitt Partners and Facing Addiction intend to help providers and payers bridge the gap and receive proper reimbursement for doing so through the Addiction Recovery Medical Home model.
RevCycleIntelligence.com recently caught up with Anne Marie Pollock, a Senior Director at Levitt Partners, to dive deeper into how the alternative payment model works and how the payments will bring value-based care to addiction recovery.
Creating a network of providers, stakeholders to engage in the APM
Before providers can receive value-based payments for addiction recovery treatment, payers and providers must come together to form a network of services, Pollock emphasized.
READ MORE: How to Prepare for Alternative Payment Model Implementation
“It's important to look at it as not necessarily any one single provider but more as an entity that has come together to be a medical home,” she said. “It requires contracts among both providers and payers, and it depends on the capacity of those willing to contract with other types of health services.”
The contracts should ultimately create a comprehensive care recovery team. The alliance intends for the care recovery team to include a peer recovery coach, primary care provider, licensed counselor, social services and community support, physical and dental specialists, and behavioral health specialists.
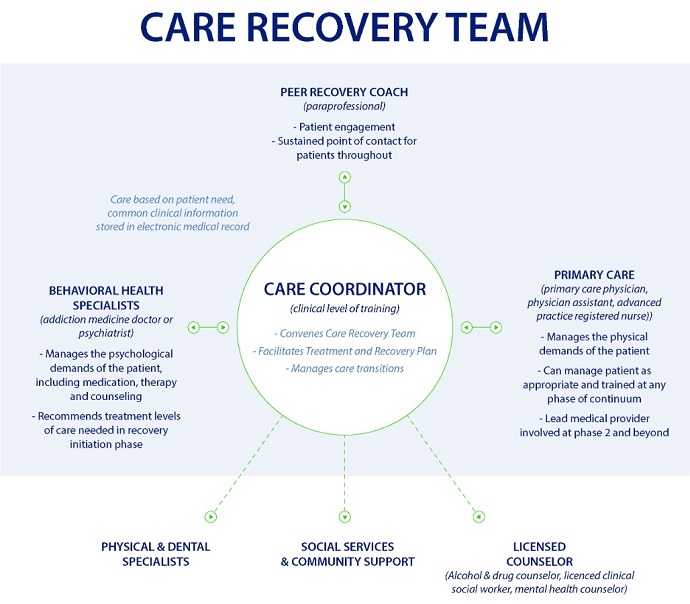
Source: Leavitt Partners, Facing Addiction with NCADD
At the center of the care recovery team is a care coordinator. The clinically-trained care coordinator will serve as the point-of-contact for the patient and providers. The individual will also coordinate the services for holistic addiction recovery treatment.
Sharing of the electronic medical record is also at the heart of the care recovery team, Pollock noted.
“We see this as a network of different types of supply chain entities and what is connecting all of them is the sharing of the electronic medical record,” Pollock elaborated. “We’ve landed on the mandatory nature of a patient consenting to share all of the records as a condition of participation because we saw it as necessary for care coordination among all of the providers.”
READ MORE: Top 5 Ingredients of a Successful Alternative Payment Model
Once the care recovery network is established, the payment component of the alternative payment model kicks in.
Value, risk-based payments for addiction recovery treatment
The Addiction Recovery Medical Home model contains three payment mechanisms that span two care episodes.
The first care episode starts once a patient agrees to be part of the medical home and undergoes pre-recovery and stabilization services, such as withdrawal management. After the pre-recovery period, which is paid via fee-for-service, the patient and providers enter the Recovery Initiation and Active Treatment episode.
The type of care provided during the first episode relies heavily on high-touch, clinical care. The episode covers the institutional spectrum, from post-emergency department inpatient care, residential treatment, to intensive outpatient care delivery, the alliance explains.
The second episode of care starts when clinicians and the patient determine that the patient can move to a more sustained recovery period in which the patient receives more community-based care. The alliance refers to the episode as the Community-Based Recovery Management episode.
“The second episode is fairly open-ended in terms of providers’ ability to contract for and pay for services for community entities,” Pollock elaborated. “The episode has a social determinants element to it, where if on a local basis a provider system thinks there is a ton of merit in contracting with a particular AA group or in contracting with a particular housing group to keep their patients in recovery and not in relapse, then they have the sub-contracting ability to do so with their episodic payment.”
The episodes are not determined by timeframes, she added. Instead the episodes are tailored to clinician and patient determinations about the level of care needed to sustain recovery. The lack of timeframe allows patients and providers to follow a personalized, high-quality addiction recovery treatment plan.
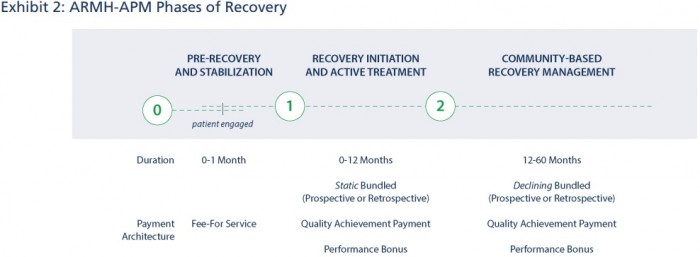
Source: Leavitt Partners, Facing Addiction with NCADD
Under the two episodes, providers in the network will receive the first type of value-based payment from payers. The payment is a blend of capitated and bundled reimbursement, Pollock explained.
“The payment is capitated in the sense that it is calibrated by patient severity,” she said. “Right now, if a patient comes in with multiple comorbid conditions or underlying behavioral or mental issues that would impact the payment.”
“And we're basing it entirely on claims history,” she added. “The claims history is the only thing we have that's set and we know how to categorize the patients by high, medium, and low severity. It’s a good place to start.”
The alliance intends to add more data sources for more accurate capitated payment adjustments.
“Over time, we hope that providers and payers will be able to identify the recovery capital, so things like housing, family presence in the area, and community support,” she stated. “These factors will be able to calibrate the severity of that patient and how likely it is that their recovery will be continuous.”
With risk-adjusted capitated payments determined, the payer will reimburse providers using the payments during each episode.
Pollock pointed out that the capitated, bundled payments are reduced for the Community-Based Recovery Management episode to reflect more community engagement. The lower payment incentivizes providers to keep their patients in community-based recovery.
“It's a financial detriment to the provider when there is a preventable recovery disruption because they don't end up getting that higher level of payment,” she said. “They stay in that episode two payment. The provider is incented financially to do everything they can to help keep the patient in recovery.”
The second type of value-based payment is layered on the bundled, capitated reimbursement. Payers will provide a quality achievement payment, or base payment, for providers who achieve care quality goals.
“The quality metrics are still under development, but the idea is the model will pay a bonus if providers score well on those metrics,” she stated. “The bonus will be determined by the contracting providers and payers.”
The National Committee for Quality Assurance (NCQA) is developing the quality metrics for the alternative payment model. The quality measures will include entry criteria, which are measures payers expect all provider to achieve, as well as outcome and process measures.
The final value-based payment type included in the alternative payment model is a shared savings performance bonus.
“The payment is sort of shared savings, shared risk between the payer and the provider involving the total claims for the individual. It will not just be the addiction health claims, but also the physical and behavioral health claims,” she explained.
“If compared to a baseline there are savings, then there are shared savings,” she continued. “A percentage goes to the physician and a percentage goes to the payer. Everyone benefits from having better care coordination and clear referrals.”
Together, the three value-based payment components will incentivize and support coordinate, holistic addiction recovery care that spans a patient’s clinical and community-based services.
The alliance of healthcare and addiction recovery groups will pilot the Addiction Recovery Medical Home model in at least two markets starting in 2019.
